🚀 We are finalizing all preparations to introduce you to the most powerful homecare software. Join the waitlist to witness something truly advanced in Summer 2025! Thank you for your interest.

See in real time what Jiris can do for you. Let the power of AI transform your agency
Get a DemoQuality home care has never been more crucial than it is today. A rapidly aging population coupled with a rising prevalence of chronic disease, has meant healthcare providers are under even more pressure to offer cost-effective and reliable services.
Unfortunately, there are a few factors standing in the way. For one, the industry isn’t free of bad-faith actors, as fraud and discrepancies continue to result in financial losses. At the same time, providers are wasting a great deal of time on administrative tasks and manual workflows while dealing with complex regulations.
In this landscape, Electronic Visit Verification (EVV) has emerged not only as a mandatory compliance requirement but also as a pertinent solution to improve patient care and caregiver accountability. Wondering how to stay compliant when selecting a homecare EVV software system? In this guide, we’ll tell you what you need to know about EVV models, touch on state requirements, and cover must-have software features required for compliance.

In 2016, the 21st Century Cures Act mandated that home and personal care providers across states implement EVV—a software solution that electronically logs crucial data about the provider’s visit in real-time. This data is parsed to ensure services are rendered as billed. To stay compliant, agencies must record data relating to:
Without proper EVV documentation, Medicaid personal care services (PCS) and home health care services (HHCS) risk claims being denied. Also, apart from its compliance benefits, access to EVV data benefits both parties. Agencies gain more oversight over their employees, improve employee retention and patients are assured about the quality of their care.
The system also eliminates the need for manual logging, which is time-consuming, inefficient, and error-prone. With EVV, home care agencies streamline documentation, scheduling, and billing—all of which indirectly improve health outcomes.
It also tackles another major issue associated with manual practices—fraud. EVV reduces instances where caregivers exaggerate time spent with patients or neglect scheduled visits altogether. If a caregiver repeatedly fails to meet service standards, the agency can take corrective action before the patient's well-being is compromised.
Consider these two stats.
When it was introduced, the Congressional Budget Office (CBO) estimated that EVV would save states $290 million over a 10-year period. Therefore, some states see financial benefits in providing reimbursements to help agencies offset the costs of EVV system implementation. Dive deep into what is EVV in homecare and why it matters.
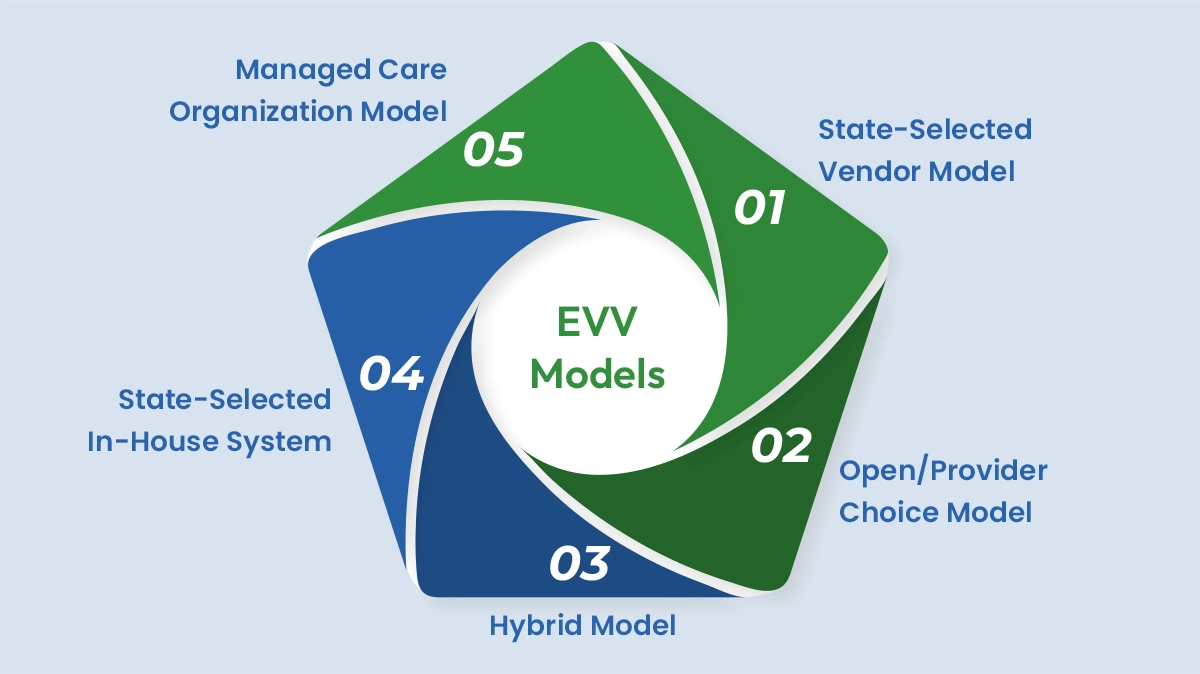
As home healthcare providers target full compliance, many EVV models have emerged, each with its own benefits, drawbacks, and requirements. Here’s a breakdown:
In this model, the state selects a specific EVV vendor for all providers to work with. This approach promotes uniformity, streamlines the sharing of data, and reduces the costs of adopting EVV systems. However, giving one vendor a monopoly over the market severely limits the flexibility and capabilities of individual providers.
Under the more flexible Open or Provider Choice model, healthcare providers can select their own EVV vendor but are responsible for its implementation and management. This gives providers access to a range of high-quality and reasonably priced solutions but also comes with a significant implementation cost.
Some states have adopted a hybrid model, which gives homecare providers the freedom to either work with a state-sponsored EVV vendor or a third-party system. By relaxing EVV home health requirements, states enable providers to find a system that is adaptable to their workflows, needs, and requirements.
However, this approach introduces complexity, as providers must ensure their EVV data integrates seamlessly with the state's aggregator. Administrative burdens increase as agencies must verify compliance on both the state and provider sides.
A state could also develop and manage its own EVV system internally. Under such a system, providers are assured state and federal compliance. However, implementation can be costly, as it requires providers to essentially adopt a whole new EVV system.
States that choose this model may benefit from better data security and control over compliance measures, but they must also manage long-term software maintenance and updates.
Under the MCO model, managed care plans are responsible for selecting the most appropriate EVV vendors for their providers. They may also cover associated costs. This approach offers versatility but can lead to inconsistencies across different providers, making standardization difficult.
While each state is mandated to have such a system in place, it can choose its own EVV for home care. A majority of the states have adopted an open or provider choice model, as it offers providers the most flexibility.
Some exceptions include Iowa, which has chosen to give managed care organizations the power to decide, or Maryland, which has a state-mandated in-house system. Check out a more detailed list of current EVV state models.
However, this is just the status as of the beginning of 2025. It’s been nine years since the 21st Century Cures Act mandated all personal care services and home health care services to implement EVV by 2021. This has proven to be a complex and painstaking process, and many states are still partially compliant, while others are figuring out the most appropriate system for its providers.
In the last few years, there has been a crackdown on homecare providers who have failed to follow the regulations. For example, last year Pennsylvania mandated an 85% compliance rate by January 1, 2025.
So, how do providers ensure EVV compliance? In an increasingly digitized world, software plays a significant role—offering providers a host of tools and features that ensure accurate tracking of services. It is important to choose the best available EVV system. Here are just some ways it helps providers.
An EVV home health software is fitted with GPS that gathers the caregiver’s location—and confirms that the service was provided at the right place, at the right time, and to the right client. Apart from being crucial for compliance, this feature significantly reduces the risk of fraudulent activity, as all claims can be verified with hard data.
EVV home care software automatically captures and records crucial data about a caregiver’s visit. This is both a crucial regulatory requirement as well as one that streamlines the healthcare agency’s documentation process. By seamlessly integrating data points into workflow, billing, and payroll models, the software allows agencies to reduce reliance on cumbersome paperwork and effectively takes human error out of the equation.
It also leaves behind an audit trail that can be used to verify or investigate discrepancies.
EVV for home health also ensures providers stay compliant with patient safety and security standards. All data is captured through secure and HIPAA-compliant processes and made available on a safe and convenient mobile app.
Furthermore, real-time tracking allows agencies to observe client visits and ensure caregivers offer quality services. Essentially, EVV doesn’t just ensure patients are safe and healthy, but that processes are compliant with crucial patient safety standards.
When implementing such a service, first look for a scalable EVV solution that seamlessly integrates with other systems and has a simplified verification process. The EVV compliant Jiris software, for instance, is ideal for both small providers and larger enterprises. With this service on your side, all you need to do is train your employees and bring all stakeholders on board to ensure seamless implementation.
The penalties for non-compliance with EVV mandates are harsh. In many cases, non-compliant agencies risk not being reimbursed for services provided or having to pay hefty fines for incorrect implementation. In certain cases, agencies could lose their licenses altogether. Additionally, failing to properly document services may result in Medicaid claims being denied, affecting financial stability. Non-compliance with EVV regulations may also open an agency up to investigations by the Medicaid Fraud Control Unit, which recovered $26.4 million from personal care services agencies in 2023.
To ensure compliance with various regulations and streamline operational efficiency, home and health care agencies need an EVV solution like Jiris.
Our customizable and HIPAA-compliant software allows agencies to streamline billing, be in charge of crucial documentation and scheduling, and reduce manual and error-prone processes. Beyond compliance, Jiris empowers agencies with enhanced caregiver tracking, fraud prevention, and real-time data access for quality assurance and better patient outcomes. Curious about how it works? Request a demo here.
AI assistant, smart shift assignment, and more. All-in-one solution for your home health agency. Our software expert will show you all features and how your organization can benefit from Jiris software.
Request your free live demo!Now it’s time to schedule your meeting
Schedule Now Need to fix your submission?Rate this article: